VANCOUVER -- As COVID-19 was spreading from care home to care home in B.C.'s Lower Mainland, infecting and killing vulnerable seniors, the Fraser Health Authority spent almost three weeks preparing a preliminary staffing plan to prevent workers from carrying the virus between facilities, according to an industry insider.
And that plan has still not been fully implemented.
It was March 26 when provincial health officer Dr. Bonnie Henry issued an order limiting staff movements between long-term care homes, something officials described as a crucially important tool in preventing new outbreaks and saving lives.
Fraser Health reacted quickly, asking care homes to submit a detailed list of employees that included, among other things, their phone numbers, professional credentials, social insurance numbers, and a note explaining whether they were taking shifts at any other facilities. The lists were to be turned in by midnight on Tuesday, March 31.
But health authority documents obtained by CTV News reveal it took until April 17, and in some cases April 18, for Fraser Health to return draft staffing assignment plans detailing which employees could work at which facilities.
And even then, the documents acknowledge "significant data gaps were identified" after the staffing assignments were sent out. In some cases, they say, "facilities received no data."
A staff leader at a private care home in the Lower Mainland, who asked not to be identified for fear of professional repercussions, said she was alarmed by how long it took to receive a staffing plan that still had not been finalized as of Thursday.
"It sends a message that they're really not taking it very seriously," she said. "I think that they have been far behind in their actions and in their planning."
The plan that was returned also contained what the insider described as a number of sloppy mistakes. She said it committed some employees to working more hours than they were actually available to work.
"(Fraser Health was) making assumptions about how many hours they thought this person could work. Well, that's not what that person can work, and that's not what we need that person to work according to our own business plan," the insider said.
"It's very strange, it's very imposing, and it's too late."
Before Fraser Health managed to deliver its draft staffing assignment, the care home had already proactively ensured that none of its employees were working at any other facilities, the staff leader said.
When the assignment eventually arrived, it included one name she didn't recognize – a care aide who had never trained nor worked at the home before.
"If you don't need them and you don't know them, that's a great way to introduce infection into the workplace," the insider said. "I don't think the risk is necessary at this point. We have a system that works. It would be more difficult than it's worth now."
As of Friday, there were still care aides working at multiple facilities in the Fraser Health region, which saw three more outbreaks at long-term care homes this week.
Eden Care Centre in Chilliwack, Guildford Seniors Village in Surrey and New Vista Care Home in Burnaby have all had a single case of COVID-19 reported so far. Officials have not indicated that shared staffing contributed to any of those infections.
On Friday, Fraser Health provided a written statement explaining that implementing Dr. Henry's order has been "a complex process that affects thousands of workers." The implementation has also been slowed because some of the data collected during the preparation of staffing assignments was "incomplete and inaccurate," according to the health authority.
"While this has delayed our timelines … we continue to work with our partners and our implementation is well underway," spokesperson Dixon Tam wrote in an email.
Fraser Health also outlined a number of other measures it has put in place in order to protect seniors from unnecessary exposure to COVID-19.
The health authority said staff working at long-term care homes or assisted-living facilities that have experienced an outbreak are immediately barred from taking shifts at other homes. In addition, once outbreaks happen, Fraser Health deploys rapid action teams that include "clinical nurse educators, infection prevention and control experts, screeners, (and) patient care quality officers supporting with communication to families."
The health authority declined to provide a timeline for when it will be able to fully implement Dr. Henry's order.
Asked this week about the lack of 100 per cent compliance by Fraser Health, B.C. Health Minister Adrian Dix said officials are doing everything in their power to protect the elderly. He also acknowledged some health authorities have been faster than others.
"Vancouver Coastal Health, which had the brunt of the original outbreak, moved quickly and is ahead of Fraser Health in terms of the transition," Dix said. "Island Health, I think, has moved quickly as well, as has Interior Health."
The minister also noted the complexity of overhauling a care home system that has relied on sharing employees between multiple facilities for decades.
"What we want to do is ensure that every seniors' home has appropriate coverage of staff," he said. "Do I want it to be faster? You bet I do, but we're getting it done with great speed."
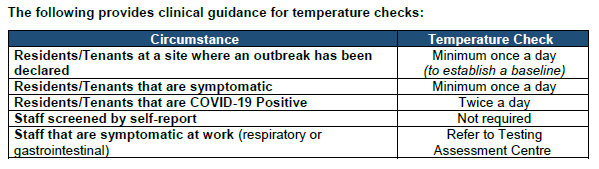
In the meantime, Fraser Health surprised some care home employees this week with a memo that appeared to recommend a relaxing of some of its precautions that were put in place for early detection of COVID-19 infections. The document, dated April 20, suggests that staff at long-term care homes and assisted living facilities are "not required" to self-screen and report their temperature if they are asymptomatic.
A number of private companies now perform temperature screening of employees before they begin work, including T&T Supermarket.
Fraser Health told CTV News it has required care home staff to be screened for fever twice per shift since March 24, and that the policy remains in place.
"Previous correspondence may have caused confusion and we are correcting," the health authority said.
This story was updated on Friday, April 24 to add a response from Fraser Health.